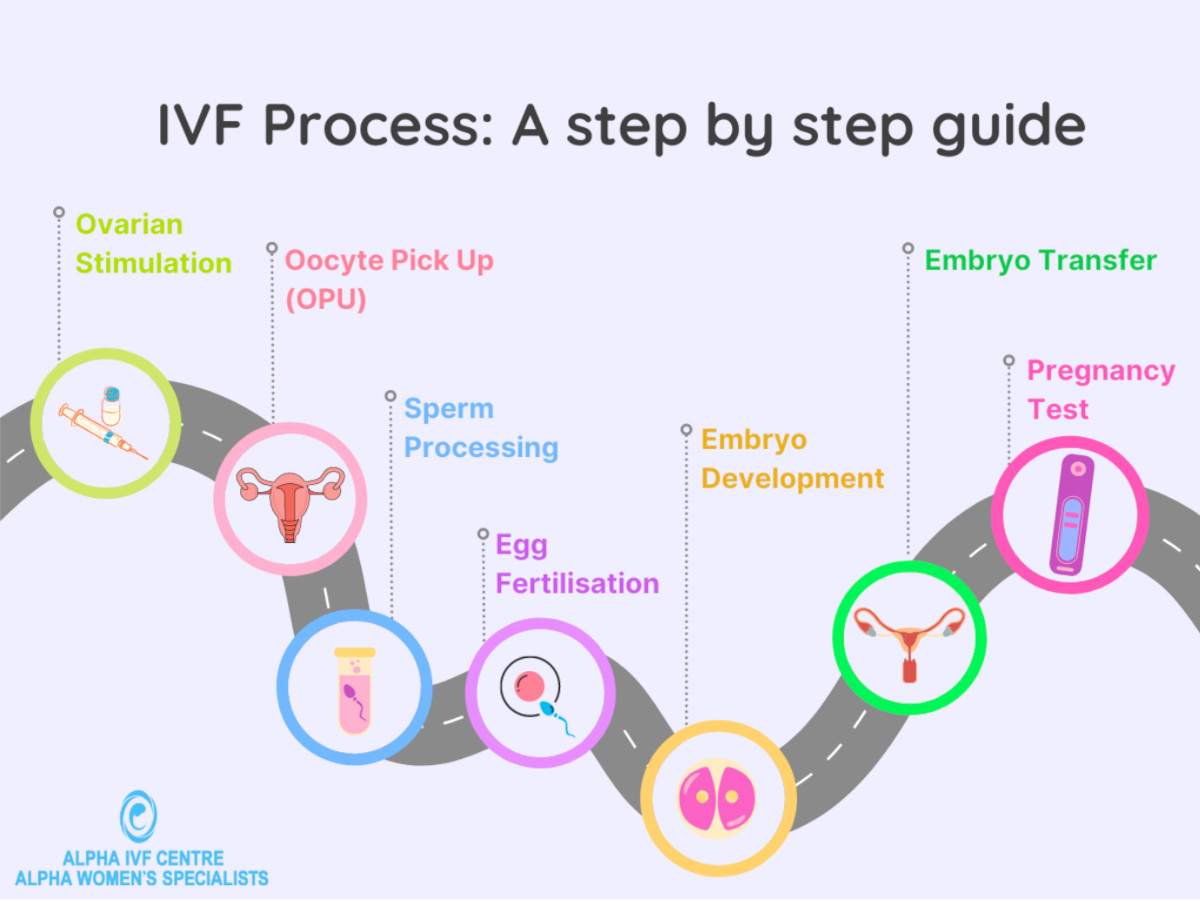
IVF overview
In-vitro fertilization (IVF) consists of a series of procedures to help couples achieve a pregnancy. The eggs are collected from the woman’s ovaries for fertilisation in the laboratory. After several days, the embryos are placed back into the uterus for implantation. A successful pregnancy is confirmed about two weeks later.
IVF is a form of assisted reproductive technology. It is offered to women with damaged fallopian tubes or when the women cannot conceive with other methods of treatment for conditions such as endometriosis, ovulatory dysfunction, unexplained infertility, and to men with sperm disorders.
Counselling and consent
As with all medical procedures, it is crucial for the couple to be counselled on the details, implications and expected results upon starting IVF treatment. Our fertility specialists, nurses, and IVF counsellor are responsible to share enough information about the procedures. The couple is encouraged to ask questions during these times. Here, a written consent of their decision to undergo the procedure is obtained.
Pre-programme preparations
Before beginning treatment, the couple is required to have their blood taken for tests on infectious diseases such as syphilis, HIV, Hepatitis B and Hepatitis C. If these tests were carried out in another country, it is still compulsory to repeat them in Singapore. A full blood count, rubella antibody test (wife) and semen analysis test (husband) may be requested by the doctor.
Ovarian stimulation
Start of IVF: Growing the follicles
The wife will undergo injections for the next 14 days or so to increase the number of eggs obtained during egg collection. These injections contain hormones that induce the growth of follicles in the ovaries (FSH and LH) and block premature ovulation (GnRH antagonist/agonist). Depending on the regime instructed by the doctor, a combination of different injections may be used.
There are two main protocols used at our centre: 1. Antagonist ‘Short’ Protocol – This is the more commonly used protocol as it involves fewer injections and is effective for most patients. Examples of GnRH (gonadotropin-releasing hormone) antagonist are Cetrotide and Orgalutran. 2. Agonist ‘Long’ Protocol – As the name suggests, this protocol requires longer days of injection. Examples of GnRH agonist are Buserelin and Leuprolide.
Semen collection & sperm preparation
The husband needs to produce a fresh semen sample on the day of egg collection at our centre. An abstinence of 3 to 5 days is advised. Should the husband feel more at ease to produce at home, please inform our nurses several days earlier to obtain a semen collection bottle. Once completed, the semen sample should arrive at our centre within an hour of ejaculation time.
Upon receiving the sample, the embryologist prepares the sperm for the fertilisation process.
Egg collection (Oocyte pick-up)
While the idea of retrieving eggs from the ovaries sounds intimidating, it’s a minor surgical procedure with little side effects and quick recovery. Sedation is given to minimise discomfort.
Under ultrasound guidance, the doctor uses a needle connected to a suction device to gently aspirate the follicular fluid of the ovaries. The embryologist then identifies and collects the eggs. It is important to note that not all follicles necessarily contain an egg and some eggs may not be mature enough for fertilisation.
The procedure takes about 15 minutes. The wife wakes up soon after and recover for a few hours before heading home.
Method of fertilisation
There are two methods in general to fertilise the eggs, namely ‘insemination’ (IVF) and intracytoplasmic sperm injection (ICSI). What separates IVF and ICSI apart is how the eggs are fertilised.
IVF insemination is the process where eggs and sperm are allowed to mix in a laboratory dish to fertilise on their own. The length of insemination can vary between a few hours to overnight, depending on the laboratory’s protocol.
ICSI is the technique that involves the direct injection of a single sperm into an egg. It is most helpful for couples with severe sperm deficiencies as it bypasses the initial steps of gamete interaction.
Embryo transfer (ET)
An embryo transfer is the last part of the IVF process. Together with the doctor, the couple will review the embryo’s development and agree on which embryo(s) to be transferred. The embryos are transferred into the uterus using a fine catheter. This is usually painless and takes only a few minutes.
The woman may go home shortly (around 30 minutes) after the embryo transfer and be given hormonal support (progesterone) to maintain the lining of the uterus and enhance chances of implantation. It is advisable not to have unprotected intercourse or high impact activities while awaiting the results.
Freezing of embryos
One may have excess good quality embryos in the IVF cycle. In this instance, these embryos can be frozen for future use, meaning there is no need to undergo another egg collection for subsequent embryo transfers. Once frozen, these embryos can be stored up to 10 years according to Singapore Ministry of Health’s regulation. There is a yearly charge for storage of these frozen embryos.
Pregnancy
The early stages of pregnancy are confirmed by a blood test on a hormone called beta-hCG, which is released by the implanted embryo. The beta-hCG blood test is usually done two weeks after the embryo transfer.
If the beta-hCG test result is positive, subsequent ultrasound scans and blood tests will be arranged to ensure that the pregnancy proceeds normally.
Disappointment and risks
There are several areas where disappointment and risks may arise, and it could be helpful for you to understand them prior to starting treatment. For example:
- Cancellation of treatment cycle due to poor follicular development
- Ovarian Hyperstimulation Syndrome (OHSS) in response to medication
- Risks of bleeding from egg collection
- Low fertilization of embryos / Poor embryo development
- Multiple pregnancies upon transfer of two embryos
- Miscarriage and ectopic pregnancies following

