In vitro fertilisation (IVF) is a widely used assisted reproductive technology (ART) that allows fertilisation of an egg with sperm outside the body. This method has enabled many individuals and couples struggling with infertility to conceive. While effective, IVF in Singapore involves several steps, and outcomes depend heavily on individual medical circumstances.
This guide outlines the IVF process, key success factors, and what to do if previous attempts haven’t worked.
The IVF Process Step by Step
The IVF journey consists of several clinical stages designed to maximise the chances of fertilisation and successful embryo implantation:
1. Ovarian Stimulation
Doctors prescribe fertility medications to stimulate the ovaries to produce multiple eggs in one cycle—rather than the single egg released naturally each month. This increases the likelihood of retrieving viable eggs.
2. Egg Retrieval
Once the eggs mature, doctors use a fine needle to collect them in a minor surgical procedure. Ultrasound guidance and mild sedation or anaesthesia ensure safety and comfort. The process usually takes 20–30 minutes.
3. Fertilisation in the Lab
Embryologists fertilise the retrieved eggs with sperm in a laboratory. If sperm quality is poor or previous fertilisation failed, they may perform intracytoplasmic sperm injection (ICSI), injecting a single sperm directly into an egg.
4. Embryo Culture
The fertilised eggs develop in a controlled incubator. Embryologists monitor them over three to five days, checking for proper development and quality.
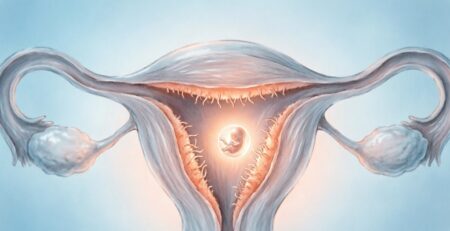
5. Embryo Transfer
Doctors select the best-quality embryo(s) and gently transfer them into the uterus using a thin catheter. Precision at this stage is vital for successful implantation.
6. Embryo Freezing (Cryopreservation)
Any remaining high-quality embryos can be frozen for future use. This allows patients to attempt pregnancy again without repeating the entire IVF cycle.
IVF Success Factors and Common Challenges
IVF remains the most effective ART method, but it doesn’t guarantee success every time. Several factors influence outcomes:
- Egg quality and quantity: Women under 35 often produce higher-quality eggs, increasing the chance of success.
- Sperm health: Fertilisation depends on sperm count, movement, and structure.
- Lab standards: A lab’s technology and quality control affect embryo viability.
- Clinician expertise: Small differences in embryo transfer technique can significantly impact results.
Approach each IVF cycle with informed expectations—results vary from case to case.
What to Do If IVF Fails
Failed IVF cycles can feel discouraging, but many patients eventually succeed. Consider the following steps:
1. Evaluate Previous Cycles
Discuss each cycle in detail with your fertility specialist. Issues such as egg quality, uterine lining, or timing could impact success. The doctor may adjust medications or try a different transfer approach.
2. Explore Additional Testing
Further tests—like hysteroscopy, endometrial receptivity analysis (ERA), or preimplantation genetic testing for aneuploidy (PGT-A)—can uncover issues and improve your next cycle’s strategy.
3. Continue With Caution
Success sometimes takes time. Many people conceive in the third, fourth, or even fifth IVF attempt. Others experience natural conception after several IVF rounds.
Practical Tips for IVF Patients
- Plan for rest: Hormonal treatments and procedures can take a toll. Allow time to recover, especially after egg retrieval and embryo transfer.
- Set realistic expectations: Not all eggs become embryos, and not all embryos implant. Each stage has its own challenges.
- Seek emotional support: Fertility treatment affects mental health. Counsellors and support groups can provide comfort and guidance.
- Track your health: Regular check-ups and hormone monitoring can help prevent side effects, such as ovarian hyperstimulation syndrome (OHSS).
Taking the Next Step
If you’re starting IVF or thinking about trying again after a failed cycle, personalisation is key. IVF works best when tailored to your individual profile. Your medical history, age, hormone levels, and previous IVF responses should all guide your next plan—not a one-size-fits-all protocol.
Speak with our fertility team today or, if you prefer remote care, explore our teleconsult service to craft a customised IVF plan that fits your health and family goals.









Leave a Reply
You must be logged in to post a comment.